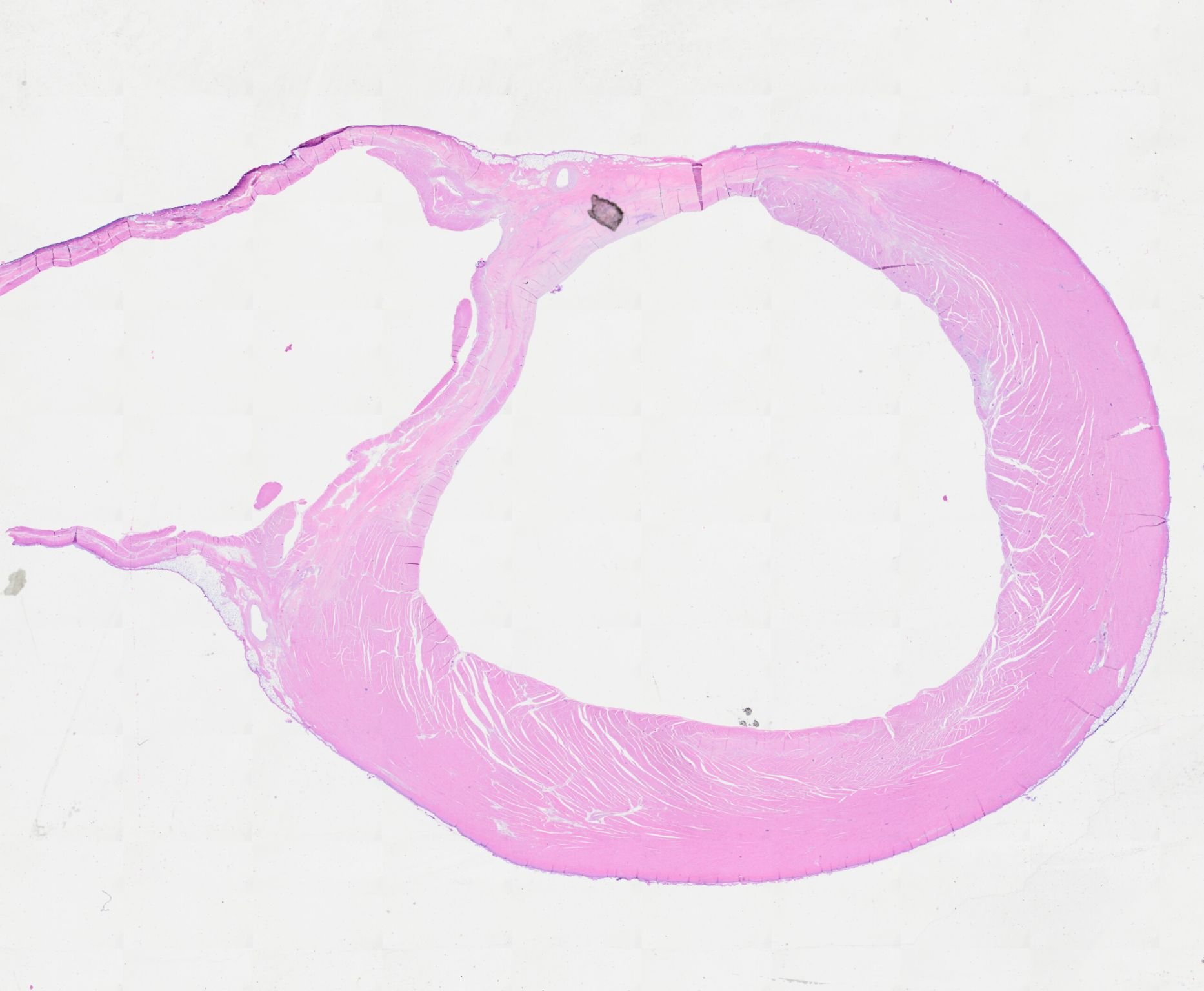
Whole-mount histological section of an ovine left ventricle with chronic scar
This image stops you for a moment. What you’re looking at is a whole-mount histological section of an ovine left ventricle with chronic scar. It is part of a project led by Anugrah Nair, supervised by Dr Poornima Balaji at Westmead Health Precinct and University of Sydney (Westmead Applied Research Centre), investigating experimental and commercially available catheter ablation energy modalities and how effectively they treat chronic ventricular scar. Out Westmead Cell Imaging Facility, led by Hui Zhang and Specialist Hong Yu have supported this with our Olympus VS200 Slide Scanner.
At first glance, it’s just pink and white architecture under a microscope. But embedded in that tissue is a very real clinical challenge. Chronic left ventricular scar, often following myocardial infarction, can form the substrate for ventricular arrhythmias. Catheter ablation is a cornerstone therapy for many arrhythmias, yet not all energy modalities create lesions of sufficient depth, durability, or precision within dense, fibrotic scar tissue. Understanding how different technologies perform in this environment is critical.
This kind of work matters for several reasons:
• It allows rigorous, side-by-side comparison of energy modalities under controlled conditions
• It helps characterise lesion depth, transmurality and tissue effects within established scar
• It provides mechanistic insight that cannot be obtained from clinical outcomes alone
• It de-risks translation before new technologies are applied in patients
Preclinical models, including ovine cardiac models, remain essential in interventional cardiology research because they allow careful histological validation of what energy delivery is actually doing at a tissue level. Clinical success is not just about delivering energy, it is about creating predictable, reproducible lesions that modify arrhythmogenic substrate safely.
Research like this sits at the interface of engineering, electrophysiology and pathology. It is meticulous, methodical and often invisible outside specialist circles. Yet it underpins safer procedures, better device development and more durable patient outcomes.
We're so grateful to see this work progressing at WIMR and to the researchers who spend hours at the bench and microscope so that therapies in the cath lab can be grounded in evidence.